Knee Replacement Infection After Surgery Is Rare.
This statement means little however if it is you who ends up dealing with an infection after surgery, one of the most serious and dreaded complications of a knee replacement.
The overall early deep infection rate for patients undergoing a primary knee replacement is 0.39%, while revision knee replacement infection rates are 0.97%.
In the first 2 years after surgery, the chance of developing an infection is estimated at 1.5%. After 2 years, the chance of infection goes down to about 0.5%.
While these numbers are exceedingly small, they are not zero, and they are only generalized statistics. YOUR individual knee replacement infection risk may be much higher so read on to find out how to lower your personal risk for one of the worst possible outcomes of knee replacement surgery.
5 Simple Steps To Lower YOUR Personal Risk of Knee Replacement Infection
 The figures above are overall national averages that can be individually influenced for better or worse by the selection of where and who does your surgery.
The figures above are overall national averages that can be individually influenced for better or worse by the selection of where and who does your surgery.
#1 Select a High Volume Hospital
Hospitals with high volumes of knee replacement surgeries have lower infection rates than small community hospitals, so pick your hospital accordingly.
#2 Select The Best Surgeon
Each surgeon will have his own rates of infection as well as overall complication rates which he’ll, no doubt, be happy to share with you… if they are lower than national averages. 😉
#3 Go Home After Surgery
If at all possible, do not hang around in places where there are more bugs. Being placed or choosing to go to a healthcare facility even briefly can negatively affect your chance of infection. No one cares more about your knee than you. Facilities have lots of foot traffic and low paid workers who may or may not be diligent about infection control. Go home as soon as possible to your own germs.
#4 Lower Lifestyle Risk Factors
Diabetes, obesity (those with BMI> 40), smoking, alcoholism, steroid use, and rheumatoid arthritis, are all well-known factors that predispose someone toward a higher risk of infection. Correcting these factors aren’t quick or easy, but try anyway. An infection is your worst outcome. Modifying your diet and lifestyle could help you head off diasaster.
#5 Optimize Nutritional Status
Diet and lifestyle will also improve your overall nutritional status which has been found to be a risk factor for infection. [7]
Malnutrition is defined by some researchers as a serum albumin level <3.5 g/dL, serum transferrin levels <200 mg/dL, and/or total lymphocyte count (TLC) <1,500 cells/mm3.
Malnutrition has been shown to interfere with optimal synthesis of collagen and proteoglycan, resulting in disruptions in the wound healing process that can lead to persistent wound drainage and increased risk of infection.
Identifying these risk factors is as easy as examining these common markers on a simple blood chemistry lab.
A recent meta-analysis revealed that hypoalbuminemia (albumin level < 3.5 g/dL) created an almost 2.5 fold increased risk of infection in generalized orthopedic surgeries. Researchers of the study recommended a “thorough nutritional consultation for each hospitalized patient in orthopedics.”[1]
In another study patients with hypoalbuminemia had a higher risk for surgical site infection, pneumonia, extended length of stay, and readmission. [2]
Researchers recommended that “future efforts should investigate methods of correcting nutritional deficiencies prior to total joint arthroplasty. If successful, such efforts could lead to improvements in short-term outcomes for patients.” [2]
The Connection Between Vitamin D and Protein Status
Let’s also look at a closely related finding. Patients with post surgical infection in the hip and knee joints show significantly lower calcium and vitamin D3 levels as well as reduced protein levels (albumin and total protein) compared with primary arthroplasty and aseptic revisions.
The vitamin D status was defined as follows:
- deficiency <20 ng/mL,
- insufficiency 20–29 ng/mL
- normal: 30–100 ng/mL
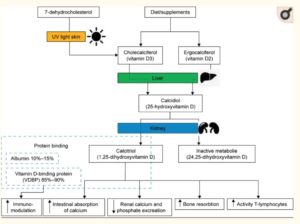
It has long been established that vitamin D deficiency has been associated with joint infections. [9] It is also known that 99% of the body’s vitamin D exists in the protein-bound form. The vitamin D-binding protein (VDBP), which serves as the most important carrier protein for vitamin D3 and its intermediates, binds about 85%–90%, while 10%–15% are bound to albumin and other lipoproteins. Less than 1% is present as unbound components of the blood. (See Chart Above). [8-9]
So we can easily conclude that reduced protein levels impact Vitamin D delivery to the cells and that all of these markers are warning signs that you have a higher risk of knee replacement infection .
Of course this scenario assumes that your surgeon provided you with this information and that he did a routine screen of your nutritional status pre-surgically to check for any problems so that you can make an informed decision.
Unfortunately, I’m not sure how prevalent pre-surgical nutritional screening is, but you have been forewarned and are now prepared.
It is something that you can ask your surgeon about and request. It is even possible to get your own testing done if none are being provided for you.
Common Causes of Low Serum Albumin
- Liver Congestion: The liver manufactures albumin. So albumin tests are often a part of liver-functioning checks. Many diseases can cause liver failure, including cirrhosis, liver cancer, hepatitis, alcohol-related liver disease, and fatty liver disease. Many livers are congested but don’t yet fall into a “disease” category.
- Kidney damage: Problems with the kidneys may cause them to release large amounts of protein into the urine. This can take albumin from the blood, leading to hypoalbuminemia.
- Protein losing enteropathy: Some stomach and gastrointestinal conditions, including celiac disease and inflammatory bowel disease, can cause the digestive system to lose a lot of protein. This causes a syndrome called protein losing enteropathy that can lead to low albumin levels.
- Low stomach acid: Hypochlorydria is another root cause of faulty protein mal-digestion because the enzymes that breakdown protein need an acid environment to start working in the stomach. Without that head start, protein may end up undigested in the intestines and unavailable for use by the cells.
- Malnutrition: People may develop hypoalbuminemia when they do not eat enough key nutrients, or medical conditions make it hard for their bodies to absorb nutrients. Some people who have recently undergone chemotherapy may be malnourished.
Albumin is present in many animal products. Changing your diet to include the following; beef, milk, cottage cheese, eggs, and greek yogurt, may improve albumin status.
If your diet already includes protein rich foods then the root problem could be in your ability to absorb, make or process the proteins.
Absorption: If you have a known GI condition or you suspect you have one, you may have trouble breaking down protein and absorbing it in the small intestine. It is best to work with a functional medicine practitioner before surgery to reduce your risk.
Processing: A congested liver may be causing the deficiency in albumin. A liver and gall bladder flush as described here could go a long way to improving your nutritional status.
Addressing vitamin D deficiency prior to surgery is essential as well. It is not possible for me to go into all the details but check here for an excellent article on symptoms and ways to reverse vitamin D deficiency.
5 Simple Steps To Lower Knee Replacement Infection Risk
- Overall knee replacement infection rates are not high but YOUR risk can be higher or lower depending on many different factors.
- Hospital and MD selection are important
- Going Home as soon as possible will lower risk
- Losing weight and quitting smoking will lower risk
- Addressing your nutritional status prior to surgery and correcting for low albumin and total protein as well as addressing vitamin D deficiency specifically 25-hydroxyvitamin D or 25(OH) D (calcidiol) will also help lower your infection risk
Resources
[1] Yuwen, Peizhi et al. “Albumin and surgical site infection risk in orthopaedics: a meta-analysis” BMC surgery vol. 17,1 7. 16 Jan. 2017, doi:10.1186/s12893-016-0186-6.
[2] Bohl, Daniel et al. “ Hypoalbuminemia Independently Predicts Surgical Site Infection, Pneumonia, Length of Stay, and Readmission After Total Joint Arthroplasty” J Arthroplasty. 31(1):15-21. Jan. 2016, doi: 10.1016/j.arth.2015.08.028.
[3] Greene, K et al. “ Preoperative Nutritional status of total joint patients. Relationship to postoperative wound complications” Journal of Arthroplasty, 6 (4); 321-5 6 Dec. 1991.
[4] Kamath AF et al. “Low Albumin Is a Risk Factor for Complications after Revision Total Knee Arthroplasty” Journal of Knee Surgery 30(3):269-275. Mar. 2017, doi: 10.1055/s-0036-1584575.
[5] Bohl, Daniel et al. “Is Hypoalbuminemia Associated With Septic Failure and Acute Infection After Revision Total Joint Arthroplasty? A Study of 4517 Patients From the National Surgical Quality Improvement Program” The Journal of Arthroplasty, 31(5): 963 – 967.
[6] Ihle C, Weiß C, Blumenstock G, et al. Interview based malnutrition assessment can predict adverse events within 6 months after primary and revision arthroplasty – a prospective observational study of 351 patients. BMC Musculoskelet Disord. 19(1):83. Mar 15 2018, doi:10.1186/s12891-018-2004-z.
[7] Gu, Alex et al. “Preoperative Malnutrition Negatively Correlates With Postoperative Wound Complications and Infection After Total Joint Arthroplasty: A Systematic Review and Meta-Analysis” The Journal of Arthroplasty, 0 (0) Jan 9, 2019, doi.org/10.1016/j.arth.2019.01.005.
[8] Zajonz, Dirk et al. “The significance of the vitamin D metabolism in the development of periprosthetic infections after THA and TKA: a prospective matched-pair analysis of 240 patients” Clinical interventions in aging vol. 13 1429-1435. 17 Aug. 2018, doi:10.2147/CIA.S171307.
[9] Zajonz D, Prager F, Edel M, et al. The significance of the vitamin D metabolism in the development of periprosthetic infections after THA and TKA: a prospective matched-pair analysis of 240 patients. Clin Interv Aging. 2018;13:1429-1435. Published 2018 Aug 17. doi:10.2147/CIA.S171307.